For individuals undergoing evaluation and treatment for brachial plexus conditions in Thrissur, understanding the steps of the brachial plexus surgery procedure can help reduce anxiety and support informed preparation. Brachial plexus surgery is a carefully planned and staged process designed to restore nerve function, improve movement, and reduce pain in the shoulder, arm, or hand. The procedure involves multiple phases, beginning well before the operation itself and continuing through recovery and rehabilitation.
1. Preoperative Evaluation and Surgical Planning
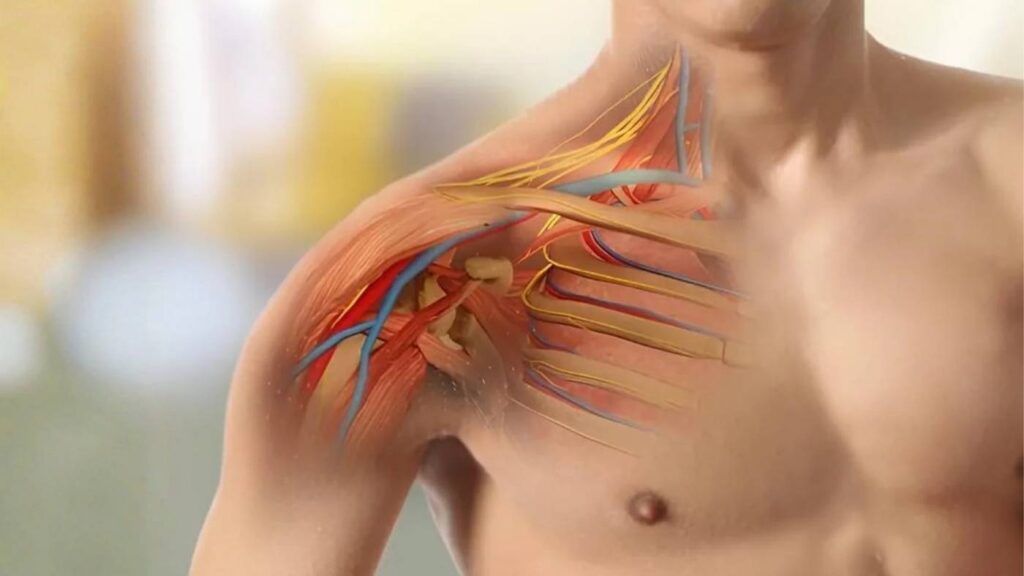
The first step in the brachial plexus surgery procedure is a detailed preoperative evaluation. This includes a thorough review of symptoms, functional limitations, and the progression of nerve injury. Clinical examination focuses on muscle strength, sensation, reflexes, and joint mobility to identify which parts of the brachial plexus are affected.
Diagnostic investigations such as imaging studies and nerve function tests are reviewed to understand nerve continuity, damage level, and surrounding tissue involvement. Based on these findings, a surgical plan is developed. This plan outlines the surgical approach, the nerves involved, and the specific techniques required. Careful planning is critical because brachial plexus surgery is highly individualized and depends on the pattern and severity of nerve injury.
2. Pre-Surgical Preparation
Before surgery, patients receive guidance on how to prepare physically and medically. This step may involve routine blood tests, imaging confirmation, and anesthesia assessment. Existing medical conditions, medications, and allergies are reviewed to ensure safety during the procedure.
Patients are also advised about fasting requirements, medication adjustments, and hospital admission details. Clear instructions are provided to help minimize surgical risks and support a smooth operative process. This preparation phase ensures that the body is ready for surgery and that potential complications are reduced.
3. Anesthesia and Positioning
On the day of surgery, anesthesia is administered to ensure comfort and immobility during the procedure. Brachial plexus surgery is usually performed under general anesthesia. Once anesthesia takes effect, the patient is positioned carefully to allow optimal access to the neck, shoulder, chest, or arm, depending on the surgical plan.
Proper positioning is essential to protect pressure points, maintain circulation, and provide clear exposure to the affected nerves. The surgical area is cleaned and prepared under sterile conditions before the operation begins.
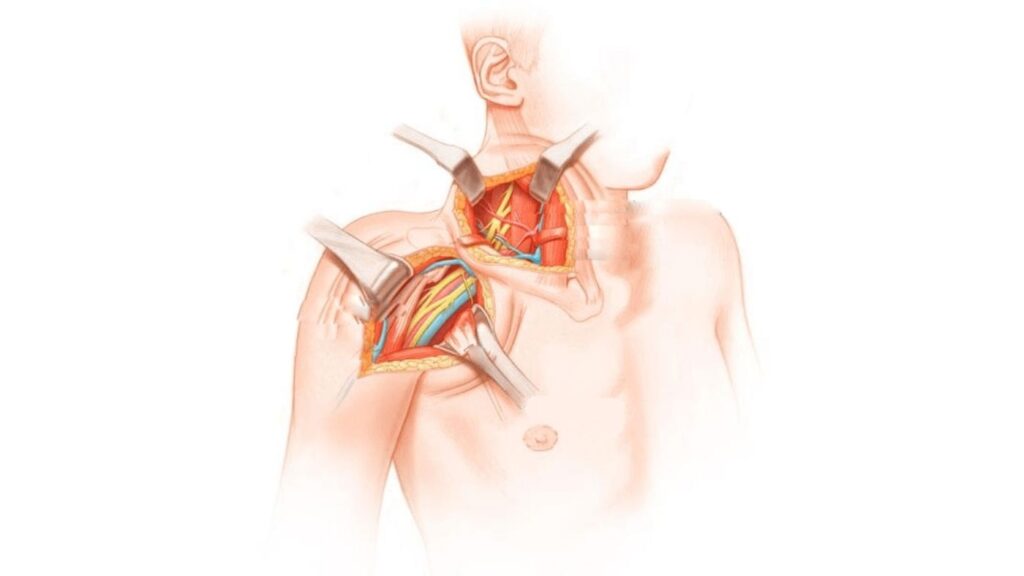
4. Surgical Exposure of the Brachial Plexus
The next step involves carefully accessing the brachial plexus. An incision is made in the planned area to expose the nerves. This step requires meticulous technique, as the brachial plexus lies close to important blood vessels and other vital structures.
Soft tissues are gently separated to identify the nerve structures clearly. This exposure allows the surgeon to directly visualize the injured nerves, assess their condition, and confirm findings from preoperative investigations. Accurate exposure is fundamental for precise nerve repair or reconstruction.
5. Intraoperative Nerve Assessment
Once the brachial plexus is exposed, the nerves are examined closely. The surgeon evaluates nerve continuity, scarring, compression, or rupture. In some cases, intraoperative nerve testing is used to assess nerve viability and functional potential.
This real-time assessment helps determine whether nerves can be repaired directly, require grafting, or need alternative reconstruction techniques. Decisions made during this step guide the choice of surgical method and influence overall outcomes.
6. Nerve Repair or Reconstruction
This is the core step of the brachial plexus surgery procedure. Depending on the type of injury, one or more techniques may be used:
Nerve repair involves reconnecting the ends of a damaged nerve when continuity can be restored without tension.
Nerve grafting is performed when a gap exists between nerve ends. A segment of another nerve is used to bridge the gap and allow nerve regeneration.
Nerve transfer involves redirecting a healthy functioning nerve to restore movement or sensation in an affected area.
The choice of technique is based on nerve damage severity, time since injury, and functional goals. Precision during this step is crucial, as nerve regeneration depends on accurate alignment and stable repair.
7. Hemostasis and Tissue Protection
After nerve repair or reconstruction, careful attention is given to controlling bleeding and protecting repaired structures. Surrounding tissues are positioned to avoid pressure or tension on the repaired nerves.
This step helps create a stable environment for nerve healing. Maintaining proper blood supply and minimizing scar formation are important for successful recovery.
8. Closure of Surgical Site
Once the nerve work is completed, the surgical site is closed in layers. Muscles and soft tissues are repositioned carefully, and the skin incision is closed using appropriate techniques.
Dressings are applied to protect the wound and reduce infection risk. The closure step marks the end of the operative phase and transitions the process into recovery.
9. Immediate Postoperative Care
After surgery, patients are moved to a recovery area for close monitoring. Vital signs, pain levels, and neurological status are assessed regularly. Pain management is initiated using medications and supportive measures.
The operated limb may be supported with slings or positioning aids to protect the surgical repair. Early postoperative care focuses on comfort, safety, and detection of any immediate complications.
10. Hospital Stay and Early Recovery
The length of hospital stay varies depending on the extent of surgery and individual recovery. During this phase, patients receive instructions on wound care, activity restrictions, and limb positioning.
Medical staff monitor healing progress and provide guidance on early movement or immobilization as appropriate. Clear discharge instructions are given to support recovery at home.
11. Rehabilitation and Physiotherapy Initiation
Rehabilitation is a critical step in the brachial plexus surgery procedure. Physiotherapy is usually started in a planned and gradual manner. Early rehabilitation focuses on maintaining joint flexibility and preventing stiffness.
As nerve regeneration progresses, therapy is adjusted to improve strength, coordination, and functional use of the limb. Rehabilitation programs are tailored to individual needs and recovery stages.
12. Long-Term Nerve Regeneration Phase
Nerve healing is a slow process. Regeneration occurs over months and sometimes years. During this phase, gradual improvements in movement and sensation may be noticed.
Regular follow-up visits are scheduled to monitor progress, adjust rehabilitation, and address any concerns. Patience and consistent therapy are important, as recovery timelines vary widely between individuals.
13. Ongoing Monitoring and Outcome Assessment
Long-term follow-up is essential to evaluate surgical outcomes. Functional improvement, pain levels, and daily activity performance are assessed during follow-up visits.
If recovery plateaus or additional issues arise, further management strategies may be discussed. Continuous monitoring ensures that recovery remains on track and that supportive care is provided when needed.
14. Functional Adaptation and Support
As recovery progresses, patients may receive guidance on adapting daily activities and protecting the affected limb. Occupational therapy may be introduced to support fine motor skills and independence.
This step emphasizes restoring quality of life and functional confidence alongside physical recovery.
Final Overview
The brachial plexus surgery procedure is a structured, multi-step process that begins with careful evaluation and continues through surgery, rehabilitation, and long-term follow-up. Each step plays an important role in supporting nerve healing and functional improvement. Understanding these steps helps patients prepare mentally and physically for the journey ahead. For individuals undergoing brachial plexus surgery in Thrissur, having a clear understanding of the procedure supports realistic expectations and active participation in recovery.
Frequently Asked Questions
1. What is the first step in the brachial plexus surgery procedure?
The first step involves a detailed preoperative evaluation, including clinical examination and review of imaging and nerve studies.
2. Is brachial plexus surgery performed under general anesthesia?
Yes, brachial plexus surgery is usually performed under general anesthesia to ensure patient comfort and safety.
3. How are the nerves assessed during brachial plexus surgery?
The nerves are carefully examined during surgery, and in some cases, intraoperative nerve testing is used to assess nerve function.
4. What surgical techniques are used in brachial plexus surgery?
Depending on the injury, techniques may include nerve repair, nerve grafting, or nerve transfer.
5. How long does the brachial plexus surgery procedure take?
The duration varies based on complexity, but the procedure often takes several hours.
6. What happens immediately after brachial plexus surgery?
After surgery, patients are monitored closely for pain control, vital signs, and neurological status.
7. How long is the hospital stay after brachial plexus surgery?
The length of hospital stay depends on the extent of surgery and individual recovery progress.
8. When does rehabilitation begin after brachial plexus surgery?
Rehabilitation usually begins gradually after surgery, starting with guided movements and exercises.
9. How long does nerve recovery take after brachial plexus surgery?
Nerve regeneration is a slow process and may take months or longer, with gradual improvement over time.
10. Is long-term follow-up required after brachial plexus surgery?
Yes, long-term follow-up is important to monitor nerve healing, functional recovery, and outcomes.
The brachial plexus is a network of nerves that controls movement and sensation in the shoulder, arm, and hand. Learn more
A good candidate for brachial plexus treatment is someone with ongoing arm weakness or paralysis from nerve injury that has not improved naturally. Learn more
The exact cost can only be determined after a detailed clinical evaluation and imaging studies, as each brachial plexus injury is unique. Learn more
Brachial plexus injuries can arise from a wide range of causes. Learn more
Common symptoms of brachial plexus injuries include weakness or paralysis of the arm, loss of sensation, nerve pain, and difficulty moving the shoulder, elbow, or hand. Learn more
Brachial plexus injuries vary in type and severity, ranging from mild nerve stretching to complete paralysis of the arm depending on which nerves are affected. Learn more
During a brachial plexus consultation, the doctor evaluates symptoms, reviews imaging and nerve studies, examines arm function, and discusses possible treatment options. Learn more
You should ask about the type of nerve injury, surgical options, expected recovery time, risks, and realistic functional outcomes. Learn more
Risks may include incomplete nerve recovery, muscle weakness, stiffness, pain, infection, or complications related to anesthesia. Learn more
Results may include gradual improvement in muscle strength, sensation, and arm function, with recovery progressing over months. Learn more
Before-and-after images typically demonstrate changes in arm position, muscle bulk, and functional improvement following treatment. Learn more