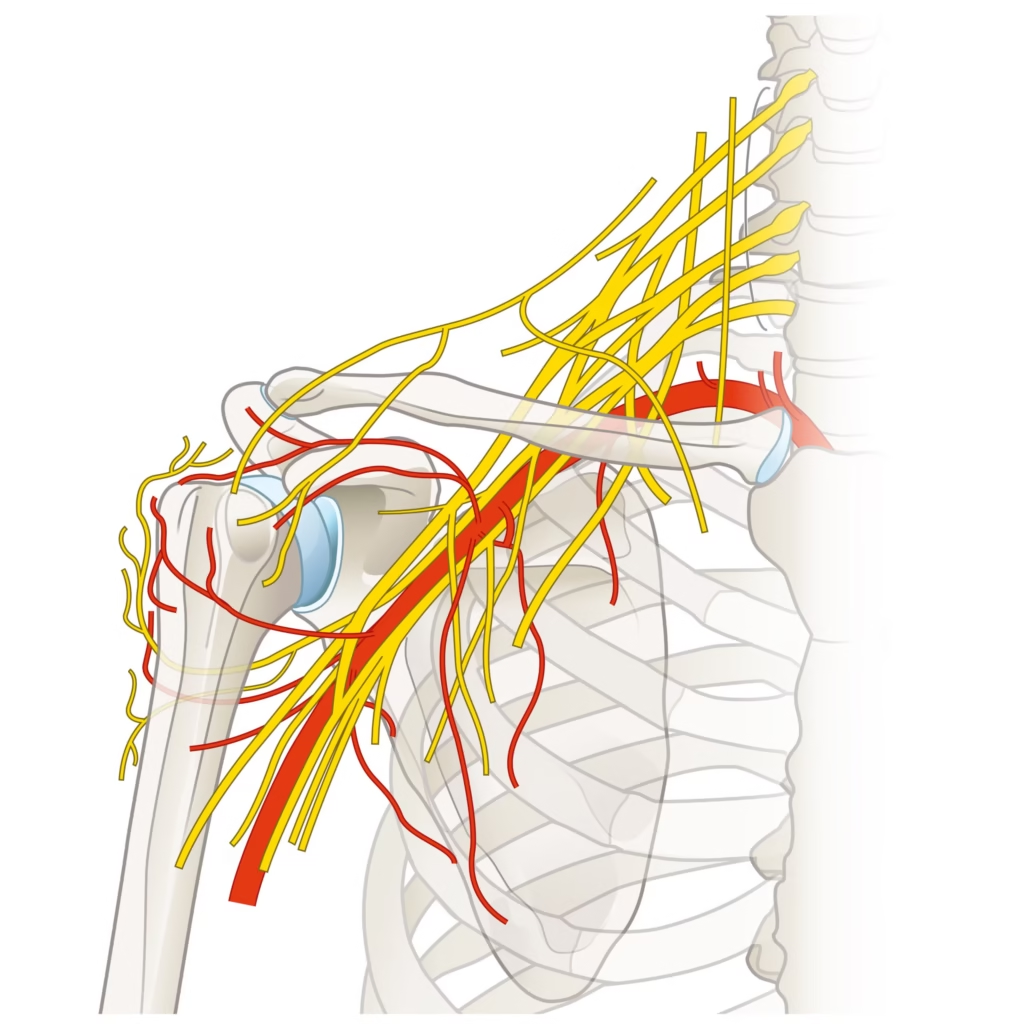
The brachial plexus is a complex network of nerves that originates from the spinal cord in the neck, specifically from the nerve roots C5 to T1, and extends through the shoulder into the arm, forearm, and hand. These nerves play a crucial role in controlling muscle movement and providing sensation to the entire upper limb. Everyday actions such as lifting the arm, bending the elbow, gripping objects, and sensing touch, pain, or temperature all depend on the proper functioning of the brachial plexus. Because of its anatomical location and complexity, this nerve network is particularly vulnerable to injury.
A brachial plexus injury occurs when these nerves are stretched, compressed, torn, or, in severe cases, pulled away from the spinal cord. Such injuries can happen due to high-impact trauma like road traffic accidents, falls from height, sports injuries, or workplace accidents. In newborns, brachial plexus injury may occur during childbirth, especially in difficult deliveries involving shoulder dystocia, prolonged labor, or excessive traction on the baby’s neck and shoulder. The severity of symptoms depends on how many nerves are involved and the extent of the damage.
Symptoms of brachial plexus injury can range from mild weakness to complete paralysis of the arm. Some individuals may experience numbness, tingling, or loss of sensation, while others may have severe nerve pain described as burning or electric shock–like sensations. Over time, untreated nerve damage can lead to muscle wasting and joint stiffness, further limiting arm function. In mild cases, where the nerves are only stretched, recovery may occur naturally over weeks or months. However, more severe injuries involving nerve tears or avulsions often require specialized medical and surgical treatment.
Diagnosis of brachial plexus injury typically involves a detailed clinical examination, imaging studies such as MRI, and nerve tests like nerve conduction studies and electromyography. These assessments help determine the location, type, and severity of the injury, which is essential for planning treatment. Management may include physiotherapy to maintain joint mobility and muscle strength, pain management, and close monitoring for signs of nerve recovery. In moderate to severe cases, advanced surgical procedures such as nerve repair, nerve grafting, or nerve transfer surgery may be required to restore function. Patients in Thrissur, Kerala and surrounding regions increasingly seek early evaluation and specialized care for brachial plexus injuries to improve functional recovery and long-term outcomes.
Early diagnosis and timely treatment are critical in brachial plexus injuries, as nerve regeneration is a slow process and delayed intervention can reduce the chances of recovery. With advances in microsurgery and rehabilitation, many patients now achieve significant improvement in arm movement and quality of life. Overall, understanding the brachial plexus and the importance of early, specialized care is key to managing these complex nerve injuries effectively.
Candidate
A good candidate for brachial plexus treatment is someone with ongoing arm weakness or paralysis from nerve injury that has not improved naturally. Learn more
Cost
The exact cost can only be determined after a detailed clinical evaluation and imaging studies, as each brachial plexus injury is unique. Learn more
Causes
Brachial plexus injuries can arise from a wide range of causes. Learn more
Symptoms
Common symptoms of brachial plexus injuries include weakness or paralysis of the arm, loss of sensation, nerve pain, and difficulty moving the shoulder, elbow, or hand. Learn more
Types
Brachial plexus injuries vary in type and severity, ranging from mild nerve stretching to complete paralysis of the arm depending on which nerves are affected. Learn more
Questions
You should ask about the type of nerve injury, surgical options, expected recovery time, risks, and realistic functional outcomes. Learn more
Consultation
During a brachial plexus consultation, the doctor evaluates symptoms, reviews imaging and nerve studies, examines arm function, and discusses possible treatment options. Learn more
Risks
Risks may include incomplete nerve recovery, muscle weakness, stiffness, pain, infection, or complications related to anesthesia. Learn more
Steps
The procedure usually involves preoperative evaluation, nerve exploration, repair or grafting, postoperative care, and structured rehabilitation. Learn more
Results
Results may include gradual improvement in muscle strength, sensation, and arm function, with recovery progressing over months. Learn more
Before and after images
Before-and-after images typically demonstrate changes in arm position, muscle bulk, and functional improvement following treatment. Learn more